A groundbreaking update to ProPublica’s investigative database, "Nursing Home Inspect," now allows the public unprecedented insight into the complex and often opaque ownership structures of American nursing homes. This development comes as research consistently demonstrates a direct correlation between the financial interests and management decisions of nursing home owners and the quality of care provided to their residents. The Centers for Medicaid and Medicare Services (CMS) data reveals a landscape where ownership is highly concentrated, with nearly one-fifth of individuals or companies reporting a financial stake in five or more facilities, and close to 100 owners controlling 50 or more homes, either directly or indirectly. This intricate web of ownership has long presented a challenge for regulators, policymakers, and the public attempting to assess accountability and ensure high standards of care for vulnerable populations.
The Critical Role of Ownership in Care Quality
The influence of nursing home ownership on the quality of resident care is a subject of growing concern and extensive academic research. Studies, such as one published in the Journal of the American Medical Association (JAMA) and referenced by sources like the National Library of Medicine, have consistently linked various ownership models, particularly private equity acquisition, to measurable changes in staffing levels, resident outcomes, and regulatory compliance. For instance, research published in Health Affairs has indicated that nursing homes owned by private equity firms tend to have lower nurse staffing levels and higher rates of health deficiencies compared to their non-private equity counterparts. These findings underscore why understanding who owns these facilities is not merely an administrative detail but a critical factor in public health and elder care.
The proliferation of multi-facility ownership further complicates this landscape. When a single individual or corporate entity controls a vast network of nursing homes, their operational strategies, financial decisions, and management philosophies can have a sweeping impact across states and diverse communities. While multi-facility ownership can theoretically lead to economies of scale and standardized best practices, it also carries the risk of systemic issues, where a flawed policy or cost-cutting measure implemented at the top can detrimentally affect thousands of residents across numerous locations. This concentration of power necessitates robust public oversight, a task made challenging by the deliberately convoluted ownership structures often employed to limit liability and obscure ultimate beneficiaries.
A High-Profile Case: Benjamin Landa and Pinnacle Multicare
The critical need for transparency in nursing home ownership has been starkly illuminated by the case of Benjamin Landa, a prominent figure in the nursing home industry. In October, Landa was nominated by then-President Donald Trump to serve as the U.S. ambassador to Hungary. This nomination brought his extensive business interests, particularly in the healthcare sector, under increased scrutiny.
ProPublica’s investigative reporting brought to light a significant development concerning Pinnacle Multicare Nursing and Rehabilitation Center, a facility co-owned by Landa. The center is currently engaged in a lawsuit against the Trump administration, an ironic twist given Landa’s nomination by the same administration. This legal battle stems from a Department of Health and Human Services (HHS) audit that identified substantial Medicare overpayments to Pinnacle Multicare, estimated to exceed $30 million. The audit findings raised serious questions about billing practices and financial stewardship within Landa’s holdings.
In response to these allegations, an attorney representing Benjamin Landa issued a statement denying any wrongdoing. The attorney attributed the issues identified in the audit to the extraordinary circumstances of the COVID-19 pandemic, arguing that nursing homes were grappling with an unprecedented crisis during the period in question. The pandemic indeed placed immense strain on healthcare facilities, leading to staffing shortages, supply chain disruptions, and increased operational costs. However, critics argue that such challenges should not excuse financial irregularities or overbilling, especially when public funds are involved and resident care could be compromised. This specific instance underscores the intricate interplay between business interests, government oversight, and the delivery of essential health services.
Unmasking the Owners: ProPublica’s Enhanced Database
Recognizing the urgent need for greater transparency, ProPublica has significantly enhanced its "Nursing Home Inspect" database. This powerful online tool, which previously allowed users to find issues identified by federal inspectors in over 14,000 facilities, now includes the crucial ability to search by owner, manager, or officer name. This update represents a monumental step forward in public accountability for nursing homes.
The new search functionality empowers users to trace all references to an individual’s or company’s name across various facilities. Furthermore, the results can be filtered by location or by the person’s specific role within the nursing home, providing a granular view of their involvement. This capability is particularly vital because, as ProPublica’s analysis demonstrates, existing public data often fails to capture the full scope of an owner’s reach.
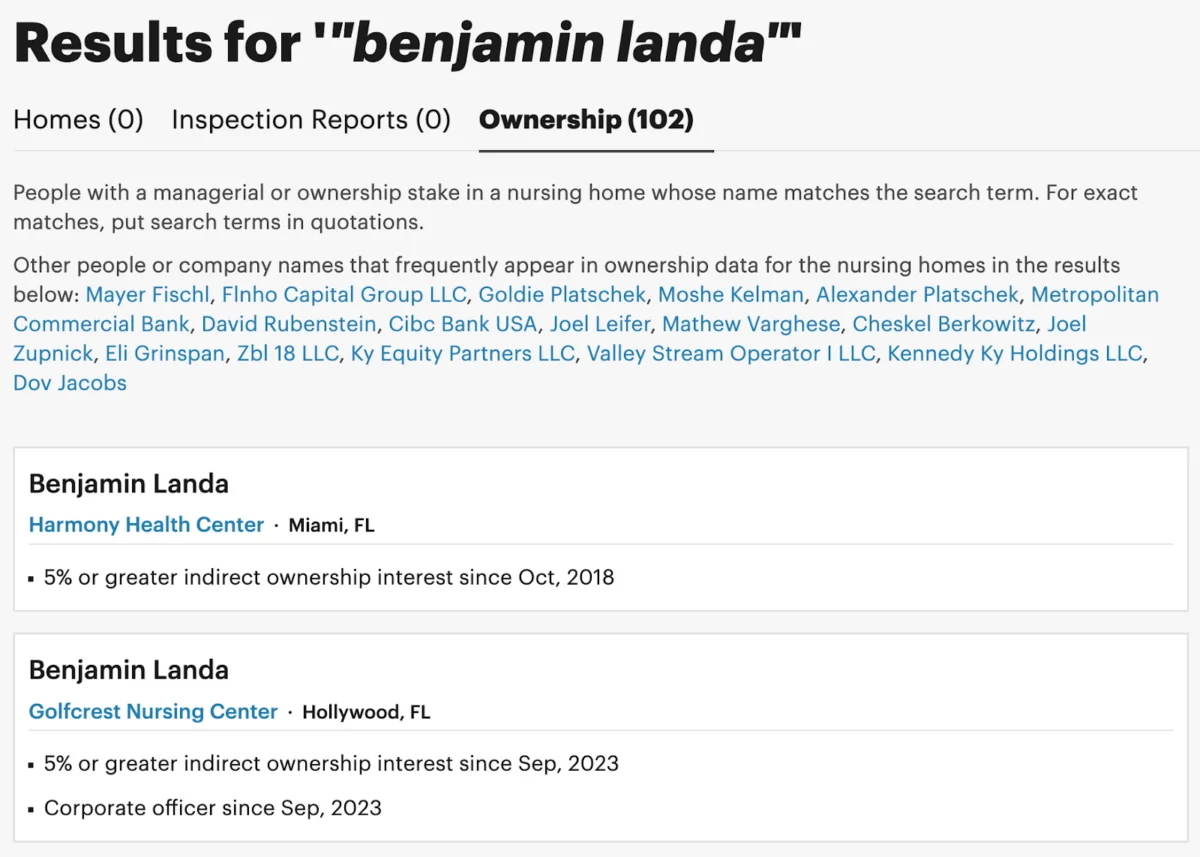
For example, while CMS data lists Benjamin Landa as an "affiliated entity" associated with 55 nursing homes across four states, ProPublica’s more comprehensive search, leveraging the full depth of CMS ownership data, reveals a far broader network. A search for "Benjamin Landa" through the updated database uncovers his name in the ownership records of 102 nursing homes spanning eight states. This disparity highlights a significant gap in previously accessible public information and underscores the importance of ProPublica’s initiative in consolidating and making this data searchable. The new tool also intelligently surfaces other individuals or companies who frequently appear alongside a searched name, helping users uncover complex partnership structures and hidden affiliations that might otherwise remain obscured. This feature is crucial for understanding who truly benefits from the operation of these facilities and where ultimate responsibility lies.

The Opaque Landscape of Nursing Home Ownership
The challenge of understanding who owns America’s nursing homes is rooted in the inherent complexity and deliberate opacity of many corporate structures. Unlike other industries where public disclosure might be more straightforward, nursing homes often operate under intricate legal arrangements involving layers of limited liability companies (LLCs), partnerships, and holding companies. These structures, while legal, can make it exceedingly difficult for regulators, journalists, and the public to identify the ultimate beneficial owners, track financial flows, and assign accountability when issues arise.
A significant trend contributing to this opacity is the increasing involvement of private equity firms in the nursing home sector. Over the past two decades, private equity acquisitions of nursing homes have surged, driven by the promise of high returns through operational efficiencies and cost-cutting measures. While proponents argue that private equity can bring capital and management expertise, numerous studies have linked private equity ownership to declines in care quality, increased regulatory violations, and higher rates of preventable hospitalizations. These firms often employ highly leveraged buyouts, burdening the acquired facilities with debt, which can then pressure operators to cut corners on staffing, supplies, and resident services to meet financial obligations. The complex financial instruments and offshore holdings sometimes associated with private equity further deepen the veil of secrecy surrounding these operations.
Regulatory Framework and Oversight Challenges
The primary federal agency responsible for overseeing nursing home quality and collecting ownership data is the Centers for Medicare & Medicaid Services (CMS). CMS mandates that nursing homes receiving federal funds (Medicare or Medicaid) disclose their ownership information. This data is then made publicly available, for instance, through the Provider Enrollment, Chain, and Ownership System (PECOS). However, as ProPublica’s findings illustrate, the way this data is collected and presented has limitations. The "affiliated entities" grouping, while useful, doesn’t always capture the full breadth of an individual’s or company’s financial interests across different legal structures or states.
Regulators face substantial hurdles in effectively monitoring such a fragmented and often deliberately convoluted ownership landscape. The sheer volume of facilities (over 15,000 nationwide), combined with the legal complexities of corporate ownership, makes comprehensive oversight a daunting task. State regulatory bodies, which are often on the front lines of inspections and enforcement, also struggle with limited resources and the challenge of navigating multi-state ownership entities. The lack of a unified, easily searchable, and fully comprehensive national database of beneficial ownership has been a persistent criticism from advocates for elder care reform. This regulatory gap creates opportunities for problematic operators to evade accountability by shifting assets, changing corporate names, or operating under multiple distinct legal entities.
Impact on Residents and Public Trust
Ultimately, the lack of transparency in nursing home ownership has profound implications for the most vulnerable members of society: the residents. When ownership is obscured, it becomes difficult for families to make informed decisions about where to place their loved ones. Without knowing the full track record of an owner across all their facilities, families might inadvertently choose a home associated with a problematic operator.
Furthermore, the opacity can hinder efforts to address systemic issues. If an owner consistently understaffs facilities or neglects maintenance across multiple homes, but their full portfolio isn’t readily apparent, it’s harder for regulators and advocacy groups to identify a pattern of misconduct and hold them accountable. This can lead to a cycle of poor care, regulatory violations, and diminished quality of life for residents. The erosion of public trust in the nursing home industry is a direct consequence of these challenges. When families hear stories of neglect, financial mismanagement, or inadequate care, and then discover that the responsible parties are hidden behind layers of corporate shell companies, it understandably fosters cynicism and fear. The ability to identify responsible parties directly is a fundamental step toward rebuilding that trust.
Looking Ahead: Calls for Greater Transparency and Accountability
The launch of ProPublica’s enhanced "Nursing Home Inspect" database is a significant milestone in the ongoing effort to bring transparency and accountability to the nursing home industry. It provides a powerful tool for journalists, researchers, policymakers, and the public to better understand the true landscape of ownership and its impact on care. This initiative aligns with broader calls for reform, including legislative efforts to mandate more comprehensive beneficial ownership disclosure across various industries, similar to measures already in place in some European countries.
Advocacy groups for seniors and patient rights organizations have long championed greater transparency, arguing that it is a prerequisite for effective oversight and quality improvement. They contend that knowing who owns a facility allows for a clearer understanding of its financial incentives, management priorities, and overall approach to care. As the U.S. population ages, the demand for nursing home care is expected to increase, making the integrity and quality of these facilities an even more pressing national concern.
ProPublica’s commitment to continuous improvement for "Nursing Home Inspect" signals an ongoing dedication to this critical issue. By inviting users to provide feedback, report issues, and suggest improvements, the investigative journalism organization is fostering a collaborative approach to enhancing public knowledge and driving systemic change. The hope is that by shining a brighter light on the hidden hands behind nursing home operations, policymakers will be better equipped to enact meaningful reforms, regulators will be more effective in their oversight, and most importantly, residents will receive the high-quality, dignified care they deserve. The ultimate goal remains to transform an often-opaque sector into one characterized by accountability, ethical practice, and unwavering commitment to resident well-being.








